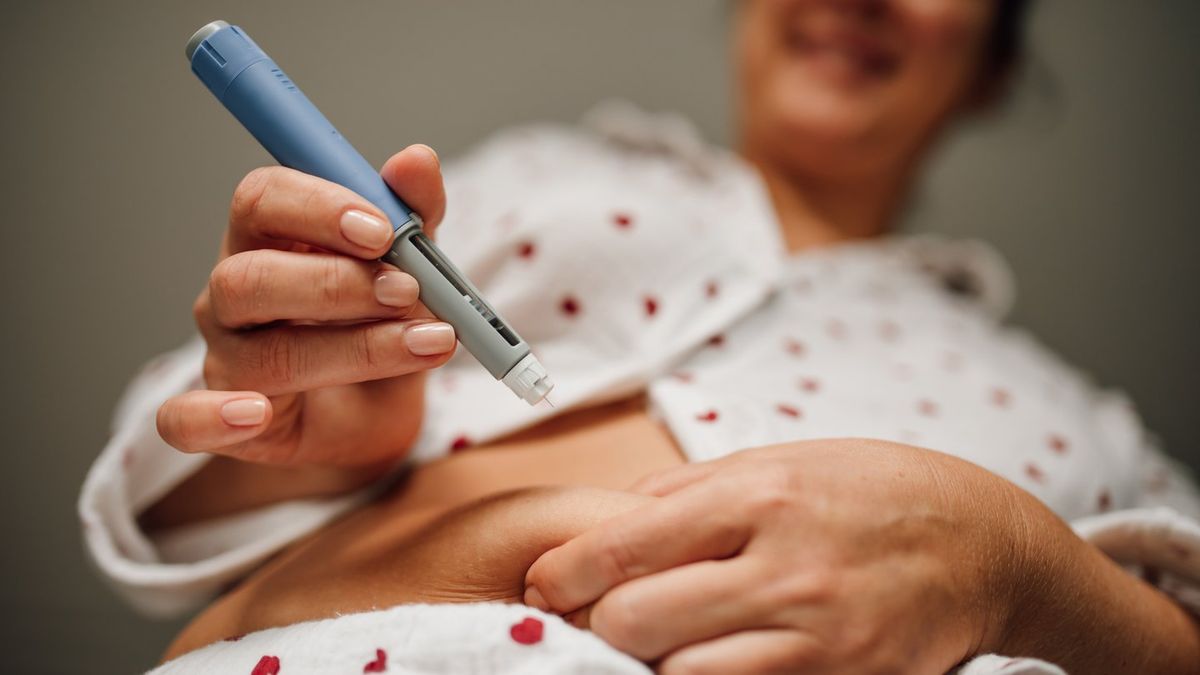
In recent years, weight-loss injections have surged in popularity, helping millions of people drop weight — including numerous celebrities who have documented dramatic changes while using medications such as Ozempic and Mounjaro.
For many users, though, the benefits can come with uncomfortable drawbacks. Commonly reported issues include nausea, vomiting, diarrhea, constipation, and abdominal pain.
Even so, demand remains high. A RAND report recently found that close to 12 percent of Americans have tried GLP-1 drugs for weight loss, including roughly one in five women between 50 and 64 years old.
Now, researchers believe a new option could eventually reduce the need to endure those side effects.
Scientists at Stanford Medicine say they’ve identified a molecule that may deliver appetite-suppressing benefits similar to today’s blockbuster drugs, but without the same unpleasant aftereffects.

The newly highlighted compound is a small peptide called BRP. It was found with the help of artificial intelligence and appears to influence the brain region that regulates hunger, potentially allowing people to eat less and lose weight without triggering nausea or muscle loss.
While BRP is described as producing effects comparable to Ozempic, it seems to work through a different — though related — biological route. Researchers say it activates distinct sets of neurons, which could make appetite and metabolic control more targeted.
Assistant professor of pathology Katrin Svensson, PhD, told Stanford Medicine: “The receptors targeted by semaglutide are found in the brain but also in the gut, pancreas and other tissues.
“That’s why Ozempic has widespread effects, including slowing the movement of food through the digestive tract and lowering blood sugar levels. In contrast, BRP appears to act specifically in the hypothalamus, which controls appetite and metabolism.”
Svensson, who led the research, is also a co-founder of a company aiming to move the discovery toward human testing, with clinical trials planned for the future.
AI was central to spotting BRP. Using computational tools, the team examined a large set of prohormones — inactive precursor molecules that can be cut into smaller pieces known as peptides. Some peptides can function like hormones, shaping processes such as metabolism across the brain and body.
The researchers said isolating something like BRP without AI would have been far more difficult. Because prohormones can be processed into many different fragments, traditional approaches can struggle to distinguish rare, biologically active peptides from the much larger pool of inactive pieces.
“The algorithm was absolutely key to our findings,” Svensson said.
So far, BRP has only been studied in animals, including mice and minipigs, where early results were encouraging. In the experiments, a single injection given before feeding cut food intake by about 50 percent within an hour.
Next, the team is working to identify exactly which receptors BRP interacts with and how that might translate to human biology. They’re also investigating ways to make its effects last longer, which could improve convenience if it eventually becomes a treatment option.
“The lack of effective drugs to treat obesity in humans has been a problem for decades,” Svensson said. “Nothing we’ve tested before has compared to semaglutide’s ability to decrease appetite and body weight. We are very eager to learn if it is safe and effective in humans.”